Of all the procedures in an interventional pain specialist's toolkit, radiofrequency ablation (RFA) is among the most misunderstood - and among the most transformative. Patients who have endured years of daily back, neck, or joint pain, often describe RFA as the treatment that finally gave them their life back. Here is a plain-language explanation of what it is, how it works, and who it is right for.
What Is Radiofrequency Ablation?
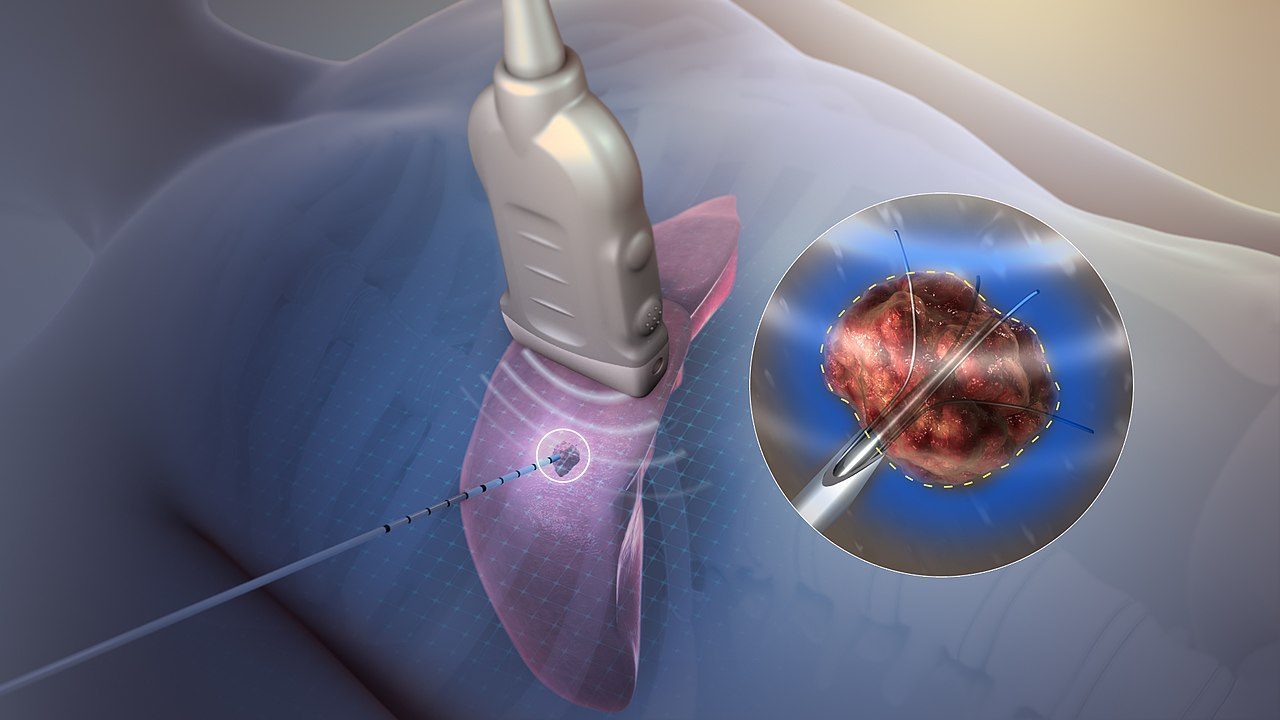
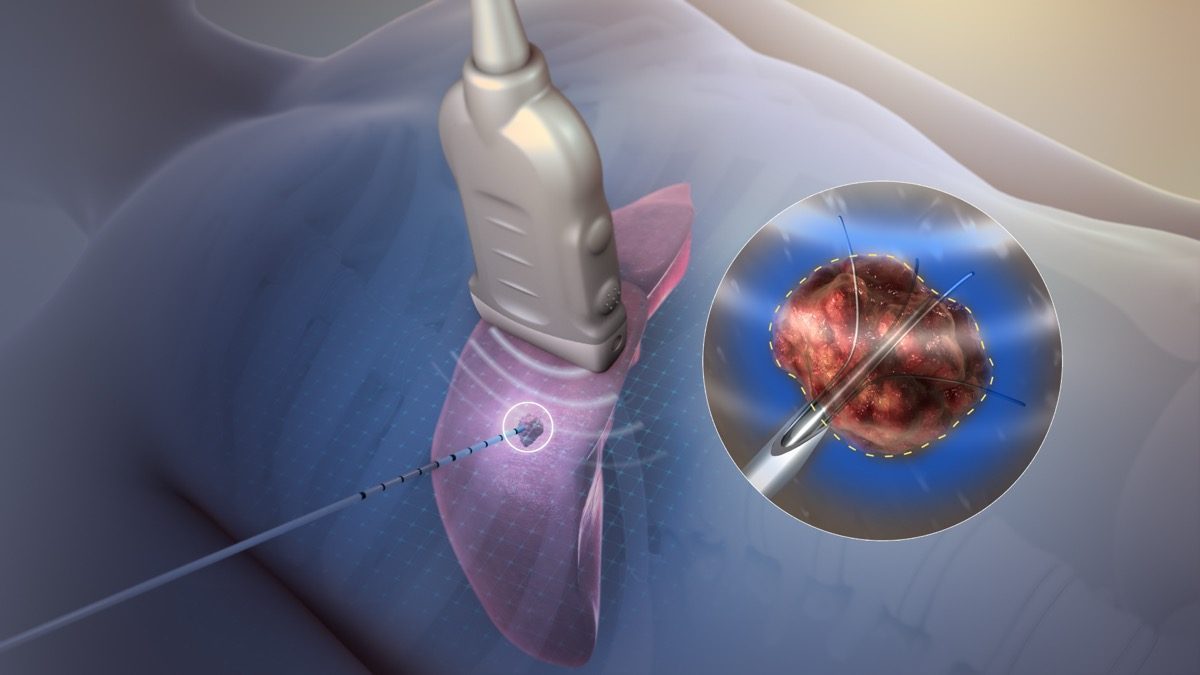
Radiofrequency ablation uses a precisely controlled electrical current to generate heat at the tip of a needle electrode. When placed next to the small nerve that carries pain signals from a specific joint - such as a spinal facet joint, sacroiliac joint, or knee joint - the heat disrupts the nerve's ability to transmit pain signals to the brain.
The nerve is not destroyed permanently. It is interrupted - effectively silenced for a period typically ranging from 12 to 24 months, sometimes longer. The joint itself is untouched; only the sensory nerve supplying it is targeted.
What Conditions Does RFA Treat?
RFA is most commonly used for pain arising from joints that are too deep or too structurally complex to treat with other means. The most frequently treated conditions include:
- Lumbar facet joint arthritis - the most common cause of axial lower back pain in adults over 40, producing aching and stiffness that worsens with extension and rotation.
- Cervical facet joint pain - a primary driver of chronic neck pain, cervicogenic headaches, and pain after whiplash injuries.
- Thoracic facet joint pain - often overlooked, responsible for mid-back pain that worsens with twisting or bending backward.
- Sacroiliac joint pain - located at the base of the spine, a significant cause of lower back and buttock pain that is frequently misdiagnosed as disc pain.
- Knee osteoarthritis - using specialised cooled RFA probes to target the genicular nerves supplying the knee, providing substantial relief for patients unfit for or unwilling to undergo knee replacement.
- Trigeminal neuralgia - severe, electric-shock-like facial pain that responds dramatically to Trigeminal Ganglion RFA when medication has failed.
At Jain Pain Clinic in Gurugram, Dr. Ashu Kumar Jain performs RFA across this full range of conditions, using both conventional and cooled RFA techniques depending on the target nerve and the anatomy involved.
The Two-Step Process: Block First, Then Ablate
A responsible RFA programme does not proceed directly to ablation. The first step is a diagnostic medial branch block - a small injection of local anaesthetic next to the target nerve. If the patient experiences significant, temporary pain relief after this diagnostic block, it confirms that the nerve in question is genuinely carrying the pain. Only then is RFA planned.
This two-step approach ensures precision. It eliminates guesswork and maximises the likelihood that ablation will produce meaningful, lasting relief.
"RFA does not mask pain - it interrupts the specific nerve circuit transmitting it. That distinction is why the relief it provides is so much more complete and durable than systemic pain medication."
What Happens During the Procedure?
The procedure is performed under real-time fluoroscopic (X-ray) or ultrasound guidance to ensure needle placement accuracy. The patient lies comfortably on a procedure table. After skin preparation and local anaesthetic, a thin radiofrequency needle is positioned adjacent to the target nerve under live imaging.
A small electrical stimulation test confirms the needle is in the correct position before the RF current is applied. The heating cycle lasts 60 to 90 seconds per nerve. Multiple nerves may be treated in the same session - for example, lumbar facet RFA typically treats three nerve levels on each side. The entire procedure takes 20 to 40 minutes, and patients are discharged the same day.
What to Expect After RFA
It is important to set realistic expectations. Some patients notice relief within a few days, but most experience the full benefit over two to six weeks as the ablated nerve fully stops transmitting. There is often some post-procedural soreness for a week, which is normal and settles with rest and mild oral analgesics.
When the nerve eventually regenerates - usually after 12 to 24 months - some patients experience a gradual return of pain. The good news is that RFA can be safely repeated when this happens, often with results as good as or better than the first treatment.
Is RFA Safe?
When performed under image guidance by a trained interventional pain physician, RFA has an excellent safety profile. The risks - which include temporary post-procedural soreness, a small chance of incomplete relief, and very rarely numbness or weakness - are far outweighed by the benefit in carefully selected patients.
Importantly, because only sensory nerves are targeted (not the motor nerves that control muscle function), RFA does not cause weakness or loss of function in appropriately selected targets.
Dr. Ashu Kumar Jain at Jain Pain Clinic in Gurugram performs radiofrequency ablation for lumbar, cervical, and thoracic facet joint pain, sacroiliac joint pain, knee osteoarthritis, and trigeminal neuralgia. If you have chronic joint or back pain that has not responded to injections or physiotherapy, RFA may be the appropriate next step.