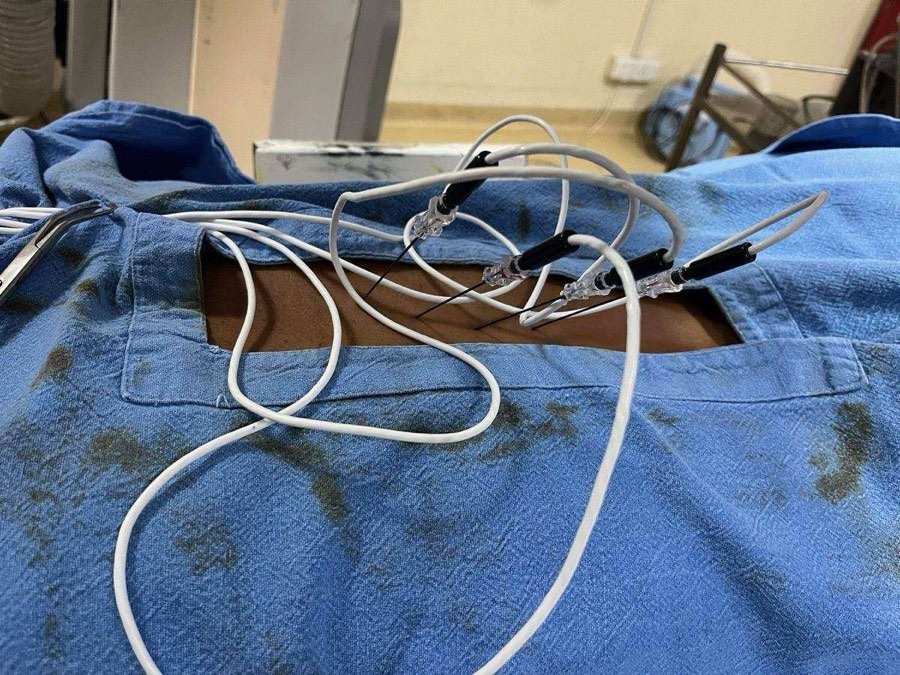
Thoracic Facet RFA
Mid-back pain from the thoracic facet joints is often overlooked and undertreated. Thoracic Facet RFA ablates the medial branch nerves at the thoracic spine, offering lasting relief for this stubborn, aching pain in the middle of your back.
Your journey
Your Road to a Pain-Free Life
Test your knowledge
How Well Do You Know This Procedure?
Frequently asked questions
What are the thoracic facet joints?
The thoracic spine has 12 vertebrae (T1–T12). At each level, paired facet joints (also called zygapophyseal joints) link the vertebrae behind the disc and guide spinal movement. Each thoracic facet joint is supplied by two medial branch nerves, small branches of the dorsal rami. When these joints become arthritic, inflamed, or strained, the medial branches carry chronic aching pain to the mid-back, often radiating parascapularly around the chest wall.
What kind of mid-back pain does Thoracic Facet RFA treat?
Thoracic Facet RFA is most effective for:
Thoracic spondylosis, degenerative arthritic change in the mid-back facet joints, often in older patients or those with a history of heavy occupational loading.
Post-thoracic surgery pain, chronic mid-back aching following spinal instrumentation surgery or thoracotomy, where facet joint irritation persists.
Thoracic facet strain, chronic pain following a mechanical injury, fall, or road traffic accident affecting the thoracic facet joints.
It is not intended for radicular pain (pain or numbness running around the chest wall in a nerve root distribution) caused by thoracic disc herniation or nerve root compression, those require a different approach.
How is Thoracic Facet RFA done?
You lie face-down on the fluoroscopy table. Under live X-ray, RF cannulas are positioned at the junction of the transverse process and superior articular process at each target thoracic level. This is the standard anatomical location for the thoracic medial branch nerve. Sensory stimulation at 50Hz confirms nerve proximity; motor stimulation at 2Hz confirms no major motor nerve is near the probe. Local anaesthetic is applied, then RF energy is delivered for 60–90 seconds per site. Multiple levels can be treated in one session. Total procedure time: 30–45 minutes.
Is a medial branch block required before Thoracic Facet RFA?
Yes. Best practice requires at least one (ideally two) positive thoracic medial branch blocks giving ≥50% pain relief before Thoracic Facet RFA is performed. These blocks confirm that the pain is genuinely originating from the thoracic facet joints and that the medial branches are the relevant pain pathway. Patients who do not respond to blocks are unlikely to achieve sustained relief from RFA.
When will I notice pain relief after Thoracic Facet RFA?
Expect mild mid-back soreness and muscle stiffness for 1–2 weeks after the procedure, the normal tissue response to heat delivered near bone. Relief then begins building as the ablated medial branch nerves progressively lose their pain-transmitting function. Most patients note meaningful improvement between 2 and 6 weeks. Full benefit is typically experienced at 6–8 weeks.
How long does Thoracic Facet RFA pain relief last?
Relief from Thoracic Facet RFA typically lasts 12–24 months. The thoracic medial branch nerves can regenerate over time, as they do in the cervical and lumbar spine. When pain returns after successful RFA, a repeat procedure can be planned. Most patients find that repeat procedures give comparable relief to the first.
How does Thoracic Facet RFA differ from Lumbar Facet RFA?
The principle is the same (medial branch ablation) but the thoracic anatomy is more complex. At thoracic levels, the medial branches lie at the junction of the transverse process and superior articular process, whereas at lumbar levels they run along the groove at the base of the superior articular process. The thoracic medial branches also have a more variable course. Fluoroscopic technique is carefully adapted for these thoracic landmarks. Additionally, the thoracic spine is less commonly a source of diagnosed facet pain than the lumbar spine, which means many patients with mid-back facet pain go unrecognised for years.
Any concern?