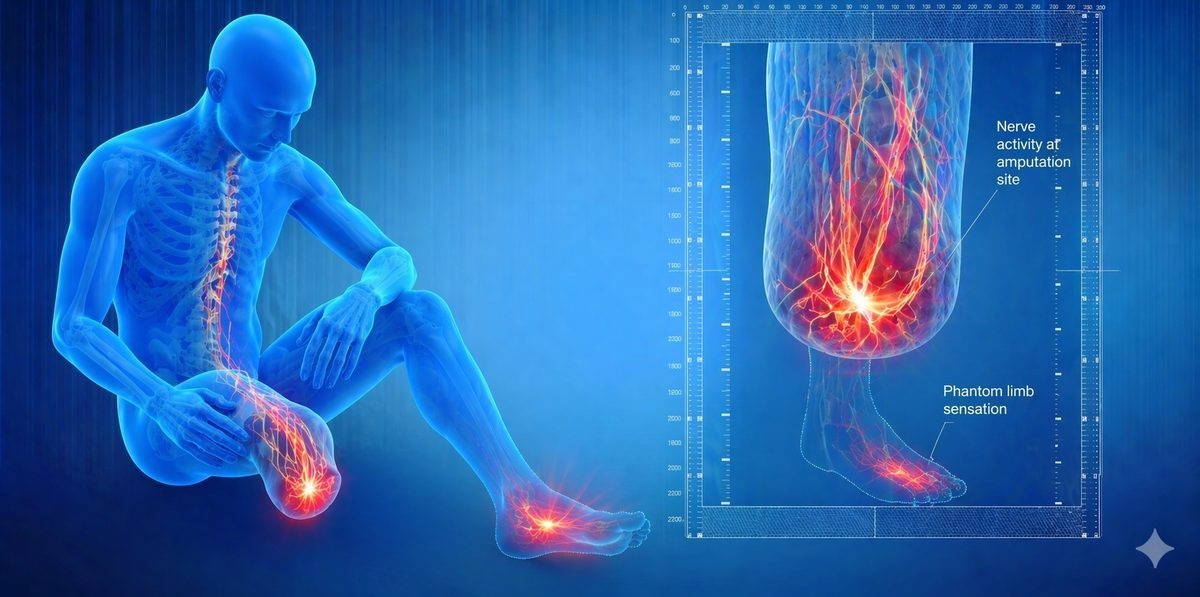
Phantom Limb and Stump Pain: Causes, Diagnosis, and Treatment
Pain felt in a limb that is no longer there is one of the most puzzling experiences in medicine. It is real, it can be severe, and with the right interventional treatment, it can be controlled.
After an amputation, a large proportion of patients continue to feel pain as though the missing limb is still present. This is not imaginary. It is driven by real changes in the nervous system. With expert interventional pain management, significant and lasting relief is possible.
What is Phantom Limb Pain?
Phantom limb pain is pain that appears to come from the part of the body that has been amputated. It can affect any amputee, whether the loss involved an arm, leg, hand, or foot.
The brain maps every part of the body in a region called the somatosensory cortex. After amputation, the nerves from the missing limb no longer send normal signals. The brain interprets this as pain. Over time, something called cortical reorganisation can make the problem worse. Nearby body parts begin to take over the brain area that used to represent the missing limb, and this remapping drives ongoing pain signals.
Phantom limb pain is different from phantom sensation, which is simply the feeling that the limb is still there without pain. Both are common after amputation. Pain affects up to 80% of amputees to some degree.

What is Stump Pain?
Stump pain, also called residual limb pain, is pain felt directly in the remaining part of the amputated limb rather than in the missing portion. It is a separate condition, though it can occur alongside phantom limb pain.
The most common cause of stump pain is a neuroma. When a nerve is cut during amputation, the cut end tries to regrow. The growing nerve fibres curl back on themselves and form a tangled, sensitive lump called a neuroma. Any pressure on the stump, such as from a prosthesis, can trigger intense pain from this neuroma.
Other causes include poor stump healing, bone spur formation, soft tissue scarring, and infection.
Symptoms of Phantom Limb and Stump Pain
The character of pain varies from person to person, but common descriptions include:
- Burning, shooting, or electric-shock like pain in the area where the limb used to be
- Cramping or squeezing sensations in the phantom limb
- A feeling that the missing limb is stuck in a painfully abnormal position
- Sharp, stabbing pain at a specific point in the stump, often worse with prosthesis use
- Constant aching in the residual limb
- Pain that worsens with touch, temperature changes, or emotional stress
- Sleep disruption caused by pain at night
Pain that interferes with prosthesis fitting or rehabilitation should always be assessed by a pain specialist. It is very treatable with the right approach.

What Causes Phantom Limb Pain?
Several mechanisms work together to produce phantom limb pain.
- Central Sensitisation: The spinal cord and brain become hypersensitive after amputation. Pain signals are amplified even when the original stimulus is no longer present. This is one of the main drivers of phantom pain.
- Peripheral Nerve Activity: The cut ends of nerves in the stump continue to fire abnormal electrical signals. These signals travel up to the brain and are interpreted as coming from the missing limb.
- Cortical Reorganisation: The brain area that used to receive signals from the amputated limb starts to be taken over by neighbouring areas. This reorganisation is associated with increased phantom pain intensity.
- Pre-amputation Pain: Patients who had severe pain in the limb before the amputation are more likely to develop phantom limb pain. The pain memory appears to be stored in the nervous system.
- Sympathetic Nervous System Activity: The sympathetic nervous system maintains a state of heightened nerve sensitivity in some patients, perpetuating phantom and stump pain.
How is Phantom Limb Pain Diagnosed?
The diagnosis is primarily clinical, based on history and description of symptoms.
- Detailed history of the amputation, pre-amputation pain, and current symptom pattern
- Examination of the stump for neuromas, tenderness, skin changes, and prosthesis fit
- MRI or ultrasound of the stump to identify neuromas or other structural causes
- Diagnostic nerve block to test whether peripheral nerve activity is driving the pain
- Quantitative sensory testing to assess the degree of central sensitisation
Check If You Need This Treatment
What we offer?
Our approach to treating phantom limb and stump pain
We use targeted procedures to interrupt the abnormal pain signals at their source, whether that is in the peripheral nerve, the sympathetic system, or the spinal cord.
-
Spinal Cord Stimulation (SCS) to modulate the abnormal central pain signals that drive phantom limb pain, providing long-term relief without medication dependence
-
Stump Neuroma Injection and RFA to diagnose and treat painful neuromas in the residual limb, reducing the abnormal peripheral signal that feeds into phantom pain
-
Epidural Steroid Injection and Epidural Infusion to reduce spinal cord sensitisation and calm the amplified pain processing at the spinal level
-
Sympathetic Nerve Block for patients where sympathetically maintained pain is a component, improving stump circulation and reducing burning pain
-
Dorsal Root Ganglion (DRG) Stimulation for precise targeting of specific nerves supplying the residual limb, particularly useful for lower limb amputees
-
Ketamine Infusion Therapy to reset central sensitisation in patients with severe, refractory phantom pain that has not responded to other approaches
Frequently asked questions
Is phantom limb pain real or psychological?
Phantom limb pain is completely real. It is caused by genuine changes in the nervous system following amputation. The peripheral nerves at the stump continue to generate abnormal signals. The spinal cord becomes sensitised and amplifies incoming signals. The brain undergoes structural reorganisation in the area that used to receive input from the missing limb. All of these changes can be measured and they produce real pain. Patients should never be told the pain is imaginary.
What is the difference between phantom pain and stump pain?
Phantom pain is felt in the part of the limb that is no longer there, such as the missing foot or hand. Stump pain, also called residual limb pain, is felt in the remaining portion of the amputated limb. Both conditions often coexist. Stump pain is frequently caused by a neuroma at the cut nerve end. The two conditions require slightly different treatment approaches, though there is significant overlap in the interventional options available.
How does spinal cord stimulation help with phantom limb pain?
Spinal cord stimulation delivers mild electrical pulses directly to the spinal cord. These pulses interfere with the abnormal pain signals travelling up to the brain. They also trigger the release of natural pain-relieving chemicals in the spinal fluid. In phantom limb pain, this approach targets the central sensitisation that keeps the pain cycle going. Many patients experience a significant and lasting reduction in pain intensity, which allows them to sleep better, use their prosthesis comfortably, and return to normal activity.
Can a neuroma be treated without surgery?
Yes. Many neuromas respond very well to image-guided injections with local anaesthetic and steroid. When pain returns after initial injection relief, radiofrequency ablation of the neuroma provides longer-lasting results by disrupting the nerve tissue generating the abnormal signals. Surgical excision is reserved for cases that do not respond to these minimally invasive options. Dr. Ashu Kumar Jain will assess whether the neuroma is the primary pain generator with a diagnostic block before recommending any definitive treatment.
Will phantom limb pain go away on its own over time?
For some patients, phantom pain reduces gradually over months to years after amputation. For many others, it persists long-term without active treatment. The longer pain is left untreated, the more entrenched the central sensitisation becomes, making it harder to treat. Early intervention produces better results. If pain is interfering with sleep, prosthesis use, or rehabilitation, a specialist assessment is recommended rather than waiting for the pain to resolve by itself.
My stump pain makes it impossible to wear a prosthesis. Can this be treated?
Stump pain that prevents prosthesis use is a very treatable condition. In most cases, a painful neuroma is the culprit. A targeted nerve block or RFA procedure can reduce this pain significantly and often allows prosthesis fitting and rehabilitation to proceed. When central sensitisation is also a factor, spinal cord stimulation or an epidural infusion programme may be added. The goal is always to get the patient back to full function with their prosthesis.
What’s the role of botulinum toxins (Butox injection) in stump pain?
Botulinum toxin (commonly known as Butox injection) can be used as a treatment for stump pain, especially when other options have not provided enough relief. It works by blocking the abnormal nerve signals and reducing muscle overactivity or spasm around the stump. This can help decrease pain caused by neuromas, nerve irritation, or muscle tightness. The effect is temporary, but many patients experience significant pain relief and improved prosthesis tolerance after the injection. The procedure is minimally invasive and can be repeated if needed, under the guidance of a pain specialist like Dr. Ashu Kumar Jain.
Any concern?