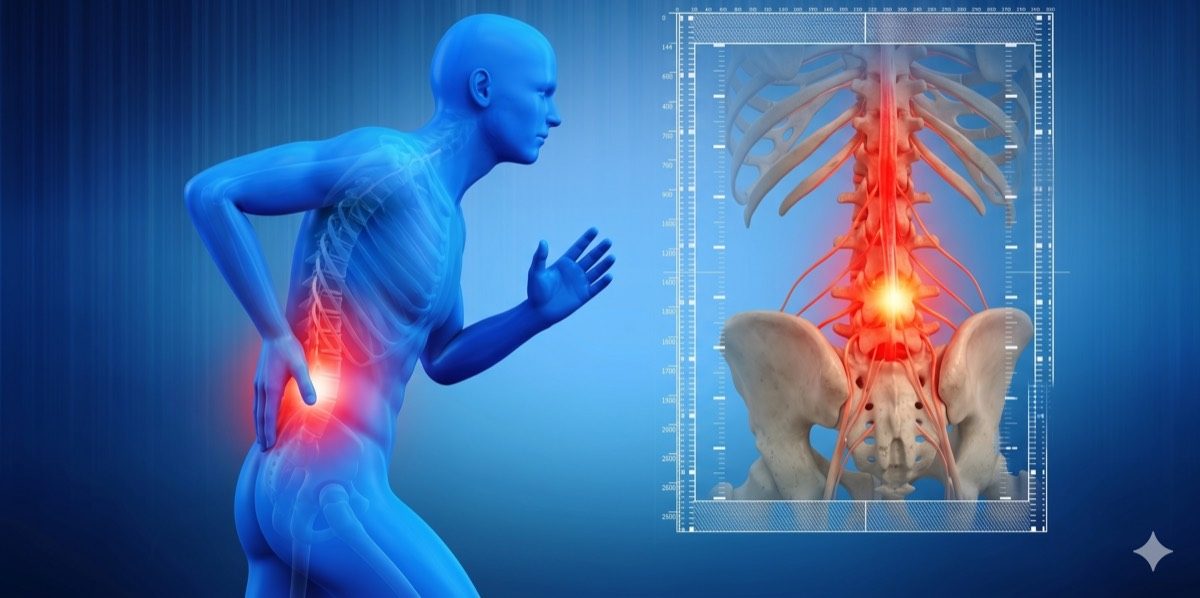
Lower Back Pain: Causes, Symptoms, and Treatment Options
Lower back pain affects millions of people and is one of the leading causes of disability worldwide. With targeted interventional treatment, most patients achieve significant and lasting relief.
The lumbar spine bears the weight of the entire upper body and is under constant stress during movement. Pain in this region can come from the discs, joints, muscles, or nerves.
What is Lower Back Pain?
Lower back pain is defined as pain felt below the ribcage and above the buttocks. It can be acute, lasting days to weeks, or chronic, persisting for more than 12 weeks.
The lumbar spine has five vertebrae, intervertebral discs, facet joints, ligaments, and an interconnected network of muscles. Damage or inflammation in any of these structures can cause back pain.
Chronic lower back pain is often caused by a combination of structural issues working together. Identifying the primary pain generator is essential for effective treatment.

Symptoms of Lower Back Pain
Symptoms vary depending on the cause, but commonly include:
- Dull or sharp pain in the lower back
- Pain that worsens with sitting, standing, or bending forward
- Morning stiffness and reduced range of movement
- Pain that radiates into the buttocks or back of the thigh
- Shooting pain down the leg if a nerve is involved
- Numbness or weakness in the leg or foot
- Pain that eases briefly with movement but returns with rest
See a specialist if back pain persists beyond 4 weeks, is severe, or comes with leg weakness, numbness, or any change in bladder or bowel function.
What Causes Lower Back Pain?
Lower back pain has many possible causes. The most common are:
- Lumbar Disc Herniation: A disc bulges outward and presses on a nerve root, causing local back pain and leg pain known as radiculopathy.
- Facet Joint Arthritis: The small joints at the back of each lumbar vertebra wear down and become inflamed, causing deep lower back pain that worsens with extension or twisting.
- Degenerative Disc Disease: Discs lose height and water content over time, reducing their shock-absorbing ability and causing chronic, diffuse back pain.
- Sacroiliac Joint Dysfunction: The joint connecting the spine to the pelvis becomes inflamed or unstable, causing pain in the lower back and buttock that is often mistaken for disc pain.
- Lumbar Spinal Stenosis: The spinal canal narrows and compresses the nerves, causing back and leg pain that typically worsens with walking and improves with sitting or bending forward.
Risk factors include a sedentary lifestyle, obesity, heavy manual work, poor posture, prior back injuries, and age-related changes in the spine.
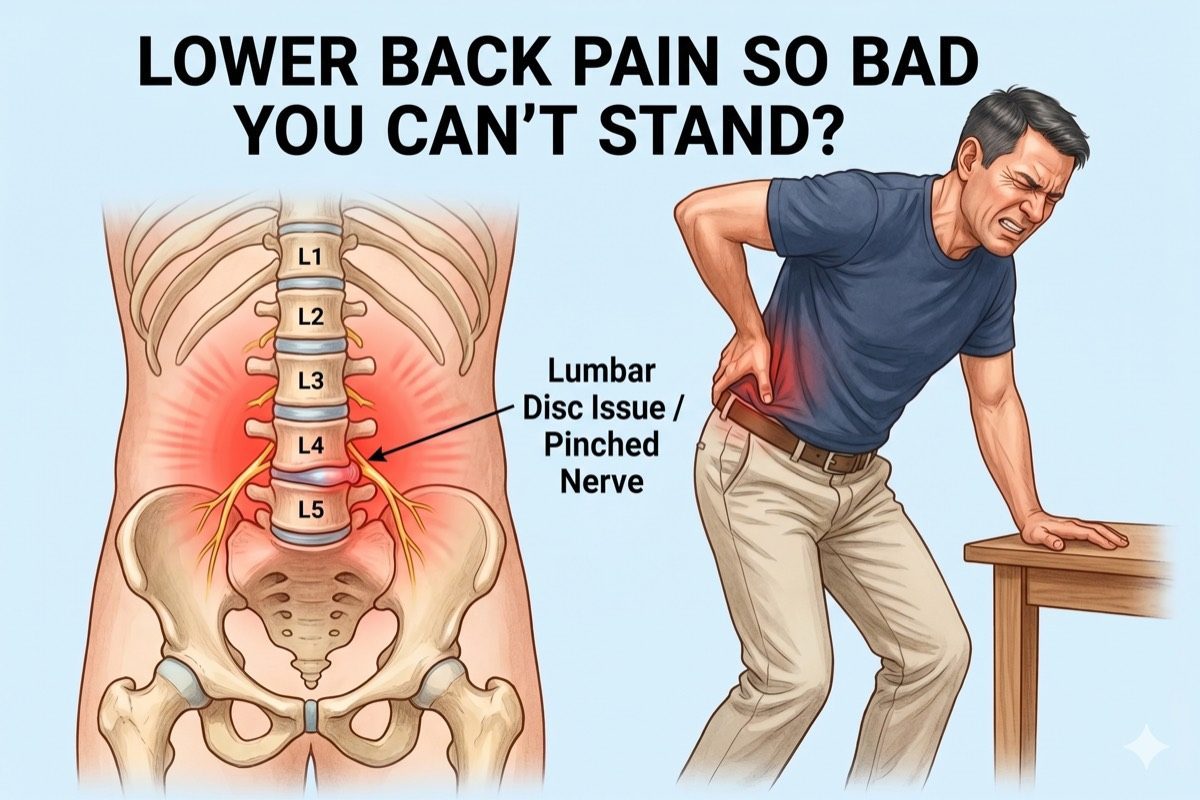
Facet Joint Pain vs Disc Pain
Not all lower back pain is the same, and the treatment differs depending on the source. Facet joint pain tends to be worse with extension (leaning back) and is usually relieved by bending forward. Disc pain is often worse with flexion (bending) and prolonged sitting.
Sacroiliac joint pain is a third common but frequently missed source. It causes pain in the lower back and buttock, often on one side, and is worse when moving from sitting to standing.
Dr. Ashu Kumar Jain uses a combination of clinical examination, imaging, and diagnostic nerve blocks to distinguish between these sources before recommending any treatment.
How is Lower Back Pain Diagnosed?
Accurate diagnosis is the first step. Back pain from different sources can feel similar, and imaging alone does not always reveal the true pain generator. Dr. Ashu Kumar Jain performs a thorough clinical assessment before ordering any tests.
- Clinical examination including posture, movement analysis, and neurological testing
- MRI of the lumbar spine to assess discs, nerve roots, and the spinal canal
- X-rays to check spinal alignment, bone spurs, and disc height
- Nerve conduction studies (EMG/NCS) for suspected lumbar radiculopathy
- Diagnostic medial branch block or sacroiliac joint injection to confirm the exact pain source
Check If You Need This Treatment
What we offer?
Our approach to treating lower back pain
We use targeted, minimally invasive procedures that go directly to the source of the pain.
-
Lumbar Epidural Steroid Injection to reduce inflammation around compressed nerve roots
-
Lumbar Medial Branch Block and Facet Joint Injection to diagnose and treat facet joint pain
-
Lumbar Radiofrequency Ablation (RFA) for long-term relief from facet joint arthritis
-
Sacroiliac Joint Injection / Cooled RFA for diagnosis and treatment of SI joint pain
-
Intradiscal Cooled RFA (Biacuplasty) for disc pain and Degenerative Disc Disease. This is one of the most advanced techniques available to help patients avoid surgery in lumbar disc disease.
-
MRI, X-ray, and nerve conduction studies for accurate diagnosis
Frequently asked questions
What is the most common cause of lower back pain?
The most common causes are lumbar disc herniation, facet joint arthritis, and sacroiliac joint dysfunction. In many chronic cases, more than one structure is involved. A proper MRI and clinical examination will identify which structure is primarily responsible for the pain.
How do I know if my back pain is from a disc or from a facet joint?
Disc pain is typically worse with bending forward and prolonged sitting, and may cause pain that runs down the leg. Facet joint pain tends to be worse when leaning back or twisting and does not usually radiate below the knee. A diagnostic nerve block can confirm the source when imaging is not conclusive.
What interventional treatments are available for lower back pain?
We offer lumbar epidural steroid injections for disc-related nerve pain, Intradiscal Cooled RFA (Biacuplasty) for disc pain and Degenerative Disc Disease, medial branch blocks and RFA for facet joint pain, and sacroiliac joint injections and Cooled RFA for SI joint dysfunction. The procedure recommended will depend on the exact source identified during your assessment.
How long does lumbar RFA last?
Lumbar radiofrequency ablation typically provides relief for 9 to 18 months. However, patients who take adequate precautions, improve their posture, manage their weight, and commit to good core strengthening exercises can experience relief of much longer duration or even permanent relief. Dr. Ashu Kumar Jain helps each patient design a personalised rehabilitation protocol suited to their individual needs.
Is bed rest helpful for lower back pain?
Prolonged bed rest is not recommended. Staying gently active and maintaining movement generally leads to better recovery than resting in bed. Short periods of rest during severe flares are acceptable, but returning to normal activity as soon as possible is important for recovery.
When should I see a pain specialist for back pain?
See a specialist if your back pain has lasted more than 4 weeks, is getting worse, or is associated with leg pain, numbness, or weakness. Seek immediate care if you experience any loss of bladder or bowel control, as this requires urgent assessment.
Is surgery always needed for a herniated lumbar disc?
Surgery is rarely needed. Most patients with a herniated lumbar disc recover well with a combination of interventional procedures including epidural steroid injections and Intradiscal Cooled RFA (Biacuplasty). Intradiscal Cooled RFA is one of the most advanced techniques available to help patients with lumbar disc disease avoid surgery entirely. Surgery is considered only when there is progressive nerve weakness or when non-surgical treatment has not provided adequate relief.
Any concern?