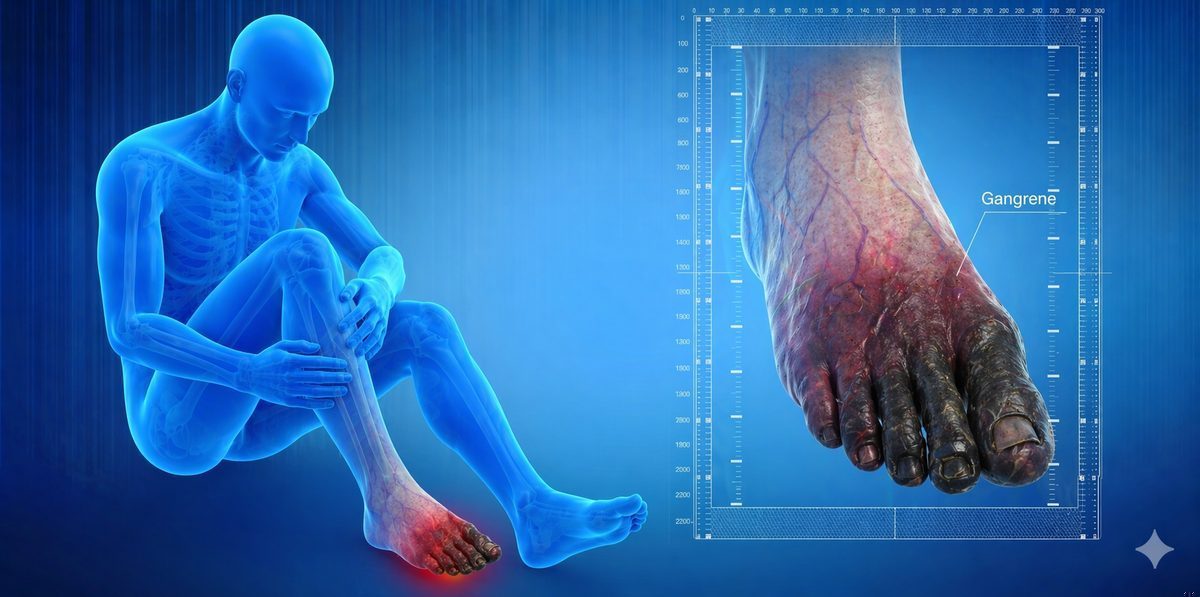
Gangrene, Buerger's Disease and Diabetic Foot: Pain Management Options
Severe limb pain from poor blood supply is one of the most distressing conditions a patient can face. Interventional pain management can reduce that pain significantly and in some cases help protect the limb.
When blood supply to a limb is severely reduced or blocked, the tissue becomes starved of oxygen. This causes intense burning pain, non-healing wounds, and in advanced cases, gangrene. Pain management plays a vital role alongside vascular treatment to protect the limb and restore quality of life.
What are Gangrene, Buerger's Disease, and Diabetic Foot?
These three conditions share a common thread. They all involve poor blood flow to the extremities, typically the feet and legs.
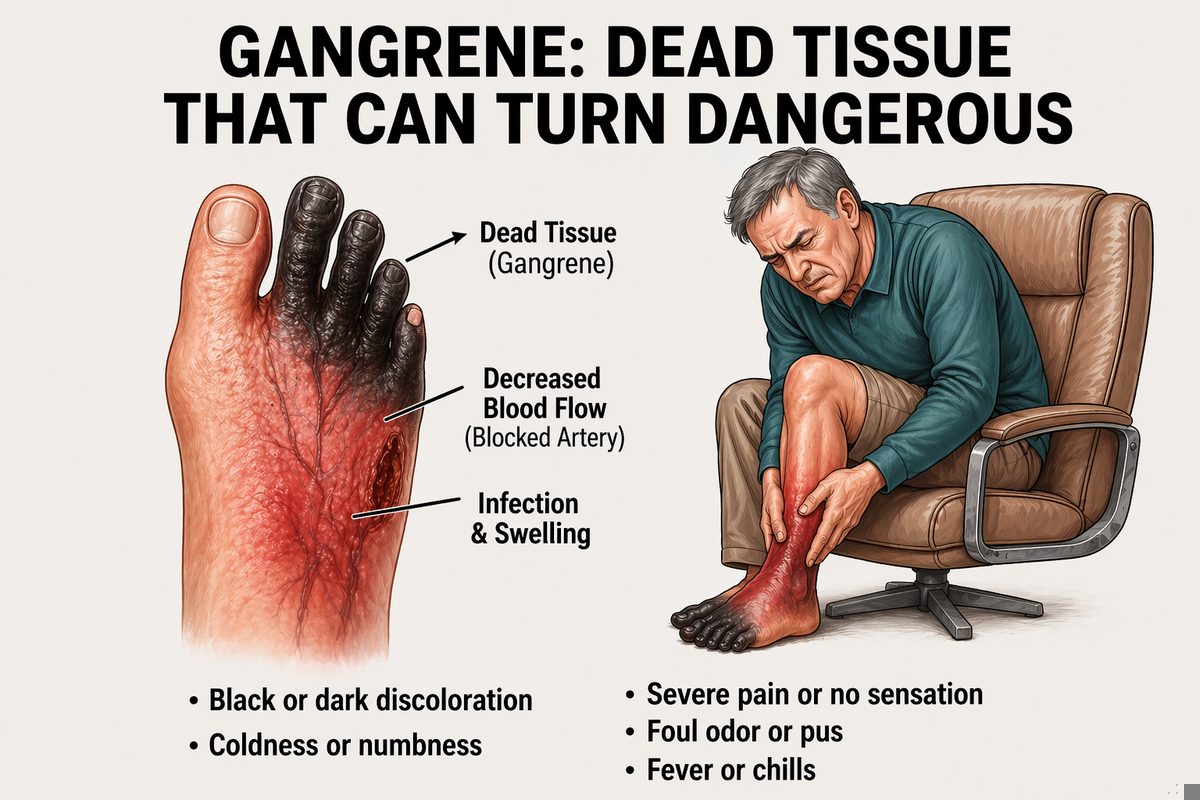
Gangrene is the death of body tissue. It occurs when blood supply is cut off long enough that cells begin to die. The affected area becomes discolored, foul-smelling, and extremely painful before sensation is eventually lost. It is a medical emergency and requires urgent treatment.
Buerger's Disease, also called Thromboangiitis Obliterans, is an inflammatory condition affecting small and medium-sized blood vessels. It is strongly associated with tobacco use. The inflammation causes clots to form inside the vessels, progressively cutting off blood flow to the hands and feet. The pain is severe and often worsens at rest, particularly at night.
Diabetic Foot is a complication of long-standing diabetes. High blood sugar damages both the nerves and the blood vessels supplying the feet. This combination of nerve damage (neuropathy) and reduced circulation (peripheral arterial disease) leads to burning pain, numbness, ulcers, and infections that are slow to heal.

Symptoms to Watch For
The early signs are easy to miss. Recognising them quickly can make a real difference to outcome.
- Burning or aching pain in the foot, toes, or calf, often worse at night
- Pain that comes on during walking and eases with rest (called intermittent claudication)
- Cold, pale, or blue-tinged skin on the feet or toes
- Skin that looks shiny and tight with loss of hair over the lower legs
- Non-healing wounds or ulcers on the feet or toes
- Numbness or tingling in the feet
- Blackening or darkening of the skin in advanced gangrene
- An unpleasant smell from infected or gangrenous tissue
Rest pain, which is pain at rest especially at night, is a warning sign that blood flow is critically reduced. This needs urgent specialist assessment.
What Causes These Conditions?
The root cause in all three conditions is compromised blood supply. The trigger differs in each case.
- Smoking: The single biggest risk factor for Buerger's disease. Smoking causes direct vascular injury and promotes inflammation and clot formation. The disease almost never progresses in patients who stop smoking completely.
- Uncontrolled Diabetes: Persistently high blood sugar damages the walls of small blood vessels and destroys the myelin sheath around peripheral nerves. Over years, this leads to the painful, complicated picture of diabetic foot.
- Peripheral Arterial Disease (PAD): Atherosclerosis narrows the arteries supplying the legs, reducing blood flow. This is particularly common in patients who smoke, have diabetes, or have high cholesterol.
- Infections: Bacteria can enter through small wounds, especially in diabetics who have reduced immunity and sensation. Untreated infection can rapidly progress to wet gangrene.
- Frostbite or Trauma: Sudden vascular injury from cold or trauma can cut off blood supply to digits and cause gangrene.
Why Does This Cause Such Severe Pain?
Pain in vascular conditions comes from multiple sources at once.
When tissues are deprived of oxygen, they release pain chemicals locally. These chemicals stimulate pain nerves in the area and cause a constant burning or aching sensation. The sympathetic nervous system, which controls blood vessel tone, also becomes overactive. This makes the vessels constrict further, worsening the ischemia and the pain. The result is a vicious cycle.
In diabetic neuropathy, the nerves themselves become damaged and start generating abnormal pain signals. This is called neuropathic pain. It is described as burning, stabbing, or electric-shock like. It is often worst at night.
Breaking this cycle is exactly where interventional pain management comes in.
How is it Diagnosed?
Accurate diagnosis helps guide the right treatment combination.
- Clinical history and physical examination including skin color, temperature, and sensation testing
- Ankle-Brachial Index (ABI) to assess blood pressure ratio between the ankle and arm as a marker of arterial disease
- Doppler ultrasound to visualise blood flow in the limb vessels
- CT or MR Angiography to map the exact location and extent of arterial blockages
- Blood tests including HbA1c (for diabetes control), lipid profile, and inflammatory markers
- Nerve conduction studies to assess the degree of peripheral nerve damage in diabetic neuropathy
- Wound culture to identify infecting organisms in ulcers
Check If You Need This Treatment
What we offer?
Our approach to treating vascular limb pain
We target the overactive sympathetic nervous system and the damaged pain pathways to reduce ischemic pain, improve circulation, and protect the limb.
-
Lumbar Sympathetic Block to interrupt the sympathetic nerves driving vasospasm, reduce burning pain, and improve blood flow to the lower limbs
-
Chemical or Radiofrequency Sympathectomy for long-lasting relief when repeated blocks confirm a good response, particularly in Buerger's disease and peripheral arterial disease
-
Spinal Cord Stimulation to improve microcirculation, reduce neuropathic pain, and promote wound healing in patients who are not candidates for vascular surgery
-
Thoracic Sympathetic Block for upper limb involvement in Buerger's disease affecting the hands and fingers
-
Epidural Infusion for short-term relief during severe ischemic pain crises and to bridge the patient to definitive vascular or sympathectomy treatment
-
Ketamine Infusion Therapy for patients with severe neuropathic pain from diabetic peripheral neuropathy that has not responded to oral medications
Frequently asked questions
What is a lumbar sympathetic block and how does it help in gangrene or Buerger's disease?
A lumbar sympathetic block is a targeted injection that numbs the sympathetic nerves running alongside the lumbar spine. These nerves control the tone of the blood vessels in the legs. When they are overactive, the vessels constrict and blood flow drops. Blocking them causes the vessels to dilate, which improves circulation to the foot, reduces burning pain, and can help heal non-healing ulcers. In Buerger's disease, this procedure is one of the most effective tools available.
Can pain management actually save a limb from amputation?
In some patients, yes. Sympathetic blocks and spinal cord stimulation improve blood flow to the affected limb. Better circulation means tissues get more oxygen, ulcers can heal, and the progression toward gangrene slows. For patients who are not candidates for bypass surgery or angioplasty, interventional pain management is often the primary treatment to preserve the limb. Results depend on how early treatment is started and the degree of arterial blockage present.
Is Buerger's disease curable?
There is no permanent cure for Buerger's disease, but it can be effectively controlled. The most important step is complete and permanent cessation of all tobacco products, including cigarettes, bidis, and smokeless tobacco. Stopping smoking halts disease progression in most patients. Alongside this, sympathectomy and other interventional procedures help manage pain and improve blood flow. With the right treatment, most patients can avoid amputation and maintain good quality of life.
My diabetic foot pain is worse at night. Why?
Neuropathic pain from diabetic nerve damage is commonly worse at night. When you lie down, there are fewer distractions, and the nervous system is in a quieter state. At the same time, blood pressure and circulation naturally drop during rest, reducing flow to an already compromised limb. This combination amplifies the burning and aching sensation. Interventional procedures that improve circulation and calm overactive pain nerves can provide significant night-time relief.
What is spinal cord stimulation and when is it used for vascular pain?
Spinal cord stimulation involves placing fine electrodes near the spinal cord. These deliver mild electrical pulses that interfere with pain signals and also stimulate the release of vasodilator chemicals. In vascular conditions, a key benefit is improved microcirculation. Smaller blood vessels in the skin and muscles dilate, increasing oxygen delivery to the affected tissue. It is recommended for patients with critical limb ischemia who have not responded to other treatments and in whom surgery is not possible.
How is gangrene pain different from other types of pain?
Gangrene pain is a mix of ischemic pain, inflammatory pain, and in some cases nerve pain. It is typically severe, constant, and burning in character. Initially the area is exquisitely tender. As gangrene progresses and tissue dies, the area may lose sensation entirely. Around the edge of the gangrenous tissue, pain often becomes even more intense. This is also known as rest pain and is a serious sign that surgical and interventional treatment is urgently needed.
Do I need surgery if I have gangrene?
Gangrene is a serious condition that requires a coordinated approach. The vascular surgeon will assess whether blood flow can be restored by bypass surgery or angioplasty. Dead tissue may need to be removed surgically. Alongside this, the pain specialist plays a critical role in controlling severe pain, improving microcirculation through sympathetic blocks, and supporting the healing process. Early presentation gives the best chance of avoiding major amputation.
Any concern?